A new controversial drug entering its next phase of clinical trials shows real promise for Alzheimer’s patients.
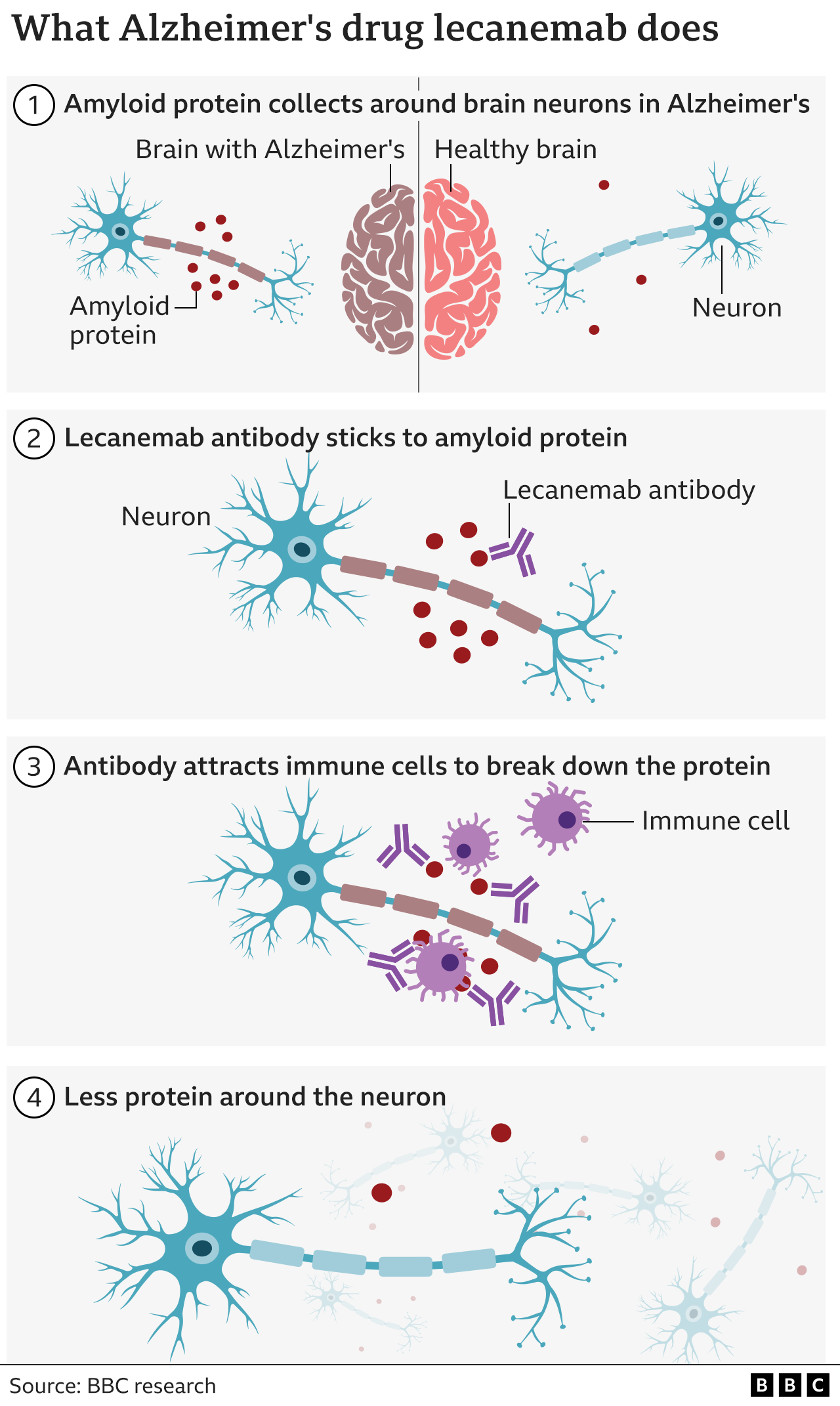
Researchers say the drug, lecanemab, is the first of its kind that is designed to actually slow, if not reverse, the processes that cause the memory-robbing disease.
Researchers and doctors alike are “cautiously optimistic” about the new drug saying it could be a major breakthrough in Alzheimer’s treatment, but it is not without some risks.

The long-awaited trial data, which was published last week in the New England Journal of Medicine, comes about two months after drugmakers Biogen and Eisai announced that lecanemab had been found to reduce cognitive and functional decline by 27% in their Phase 3 trial.
It is the first drug that has been shown to reverse or reduce dementia symptoms; other drugs used to treat Alzheimer’s thus far, have been able to slow the build-up of plaque in the brain, and slow the progression of the disease, but did not show a return of function.
The Alzheimer’s Association said in a statement that it welcomes and is further encouraged by the full Phase 3 data.
“These peer-reviewed, published results show lecanemab will provide patients more time to participate in daily life and live independently. It could mean many months more of recognizing their spouse, children, and grandchildren. Treatments that deliver tangible benefits to those living with mild cognitive impairment (MCI) due to Alzheimer’s and early Alzheimer’s dementia are as valuable as treatments that extend the lives of those with other terminal diseases,” it says.
Based on the Phase 3 results, “lecanemab has the potential to make a clinically meaningful difference for people living with the early stages of Alzheimer’s disease and their families by slowing cognitive and functional decline,” Dr. Lynn Kramer, chief clinical officer of Alzheimer’s disease and brain health at Eisai, said in a news release.
However, there were those in the trial that experienced “adverse effects.”
About 6.9% of the trial participants in the lecanemab group discontinued the trial due to adverse events, compared with 2.9% of those in the placebo group. Overall, there were serious adverse events in 14% of the lecanemab group and 11.3% of the placebo group.
The most common adverse events in the drug group were reactions to the intravenous infusions and abnormalities on their MRIs, such as brain swelling and brain bleeding called amyloid-related imaging abnormalities, or ARIA.
Some people who get ARIA may not have symptoms, but it can occasionally lead to hospitalization or lasting impairment. And the frequency of ARIA appeared to be higher in people who had a gene called APOE4, which can increase the risk of Alzheimer’s disease and other dementias. ARIA “were numerically less common” among APOE4 noncarriers, the researchers wrote.
The company aims to file for approval of the drug in the United States by the end of March, according to its news release. The US Food and Drug Administration has granted lecanemab “priority review.”
“If and when this drug is approved by the FDA, it will take clinicians some time to be able to parse out how this drug may or may not be effective in their own individual patients,” especially since carriers of the APOE4 gene could be at higher risk of side effects, said Dr. Richard Isaacson, adjunct associate professor of neurology at Weill Cornell Medicine, who is not involved in studying lecanemab or its development.
“While this study is certainly encouraging, how this translates to clinical practice, real-world clinical practice, remains to be seen,” he said of the Phase 3 trial data.
Perhaps the best news to emerge from the trial is that it proves at least that Alzheimer’s can indeed be treated, and it opens the door to other such treatments.